|
Magnesium has an effect on more than 300 bodily chemical reactions. This includes maintaining heart health, sustaining blood vessels, boosting and maintaining energy levels, producing new cells and proteins, and enabling enzyme activity.
MSM (MethylSulfonylMethane) is an abbreviation of methylsulfonylmethane, an organic form of sulfur. The chemical formula of MSM is CH3SO2CH3. It is the form in which sulfur is biologically active and appears in nature in all living organisms.
$39.95
|
|
Cancer Screening >
Breast Cancer Screening
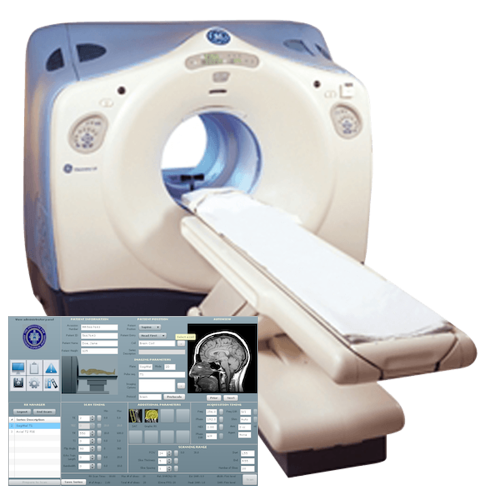
 Breast Cancer ScreeningWhat is breast cancer screening?Screening examinations are tests performed to find disease before symptoms begin. The goal of screening is to detect disease at its earliest and most treatable stage. In order to be widely accepted and recommended by medical practitioners, a screening program must meet a number of criteria, including reducing the number of deaths from the given disease. Screening tests may include laboratory tests to check blood and other fluids, genetic tests that look for inherited genetic markers linked to disease, and imaging tests that produce pictures of the inside of the body. These tests are typically available to the general population; however, an individual's needs for a specific screening test are based on factors such as age, gender and family history. In breast cancer screening, a woman who has no signs or symptoms of breast cancer undergoes a breast examination such as:
Supplemental Breast Cancer ScreeningMany studies have shown that ultrasound and magnetic resonance imaging (MRI) can help supplement mammography by detecting breast cancers that may not be visible with mammography. Neither MRI nor ultrasound is meant to replace mammography. Rather, they are used in conjunction with mammography in selected women. Women should consult with their referring doctor or radiologist to determine if MRI or ultrasound screening is appropriate for them.
Who should consider breast cancer screening – and why?About Breast CancerBreast Cancer is cancer that forms in tissues of the breast, usually in the ducts (tubes that carry milk to the nipple) and lobules (glands that make milk). It occurs in both men and women, although male breast cancer is rare. Breast cancer is the second leading cause of death from cancer in American women. About one woman in eight will be diagnosed with the disease over the course of her lifetime. A woman's risk of developing breast cancer increases with:
Women at high risk for breast cancer include those who have:
Screening RecommendationsAlthough guidelines differ, major regulatory bodies agree that annual screening mammography starting at age 40 saves lives. According to the U.S. Department of Health and Human Services (HHS), women between the ages of 40 and 74 who have screening mammograms have a lower chance of dying from breast cancer than women who do not. Screening mammography is recommended every year for women who are at average risk for breast cancer beginning at age 40 by the American College of Radiology (ACR) and the Radiological Society of North America (RSNA). The American Cancer Society (ACS) recommends that women aged 40-44 talk to their doctor and consider screening, which saves lives. Per ACS, screening mammography should begin at age 45 and be done every year until age 55 after which women can transition to every other year. The United States Preventive Services Task Force (USPSTF) recommends that regular screening mammography for average risk women should begin at age 50 and be done every other year. The National Cancer Institute (NCI) advises women who have had breast cancer and those who are at increased risk due to a family history of breast cancer to seek expert medical advice about the frequency of screening and whether they should begin screening before age 40. The age at which screening mammography should stop has not been firmly established but in general, it is thought that screening should continue as long as a woman is in good health regardless of age. Women at high risk for breast cancer should follow different guidelines. According to American Cancer Society guidelines, most women at high risk should begin screening with MRI and mammography at age 30 and continue for as long they are in good health. Some women at high risk may begin MRI screening at age 25. It is important to remember that most breast cancer occurs in women with no risk factors. Women should see their radiologist or primary care doctor to determine when to begin and how often to undergo breast cancer screening. How is breast cancer screening performed?Clinical Breast Exam In a clinical breast exam, the doctor carefully feels the breasts and underarm area for lumps or anything else unusual. Women may also perform a breast self-exam by checking their own breasts for lumps or changes in size or shape. The clinical breast exam and breast self-exam can help women become more familiar with the regular look and feel of their breasts and more readily identify changes. Screening Mammography Mammography is a type of x-ray examination used to examine the breasts. This type of imaging involves exposing the breasts to a small amount of radiation to obtain pictures of the inside of the breasts. During mammography, a specially qualified radiologic technologist will position your breast in the mammography unit. Your breast is placed on a special platform and compressed with a paddle (often made of clear Plexiglas or other plastic). The technologist will gradually compress your breast and while you hold still. Usually two images of each breast will be obtained an image producing a top-to-bottom view of the breast and an image producing an angled side-to-side view. Breast Tomosynthesis Breast tomosynthesis, also called three-dimensional (3-D) mammography, is an advanced type of breast imaging that uses low-dose x-rays and computer reconstruction to create images of the breast. It aids in the early detection and diagnosis of breast cancer before women experience symptoms. Breast tomosynthesis is not yet available in all imaging facilities. Breast Ultrasound Breast ultrasound is a type of imaging that uses sound waves to create pictures of the inside of the breast. Breast ultrasound can capture images of areas of the breast that may be difficult to see with mammography. It can also help to determine whether a breast lump is a solid mass or a fluid-filled cyst. For breast ultrasound, you will lie on your back on the examining table. A clear water-based gel is applied to your breast and the sonographer (ultrasound technologist) or radiologist will then press the transducer firmly against your skin, sweeping over the breast. Breast MRI During breast MRI, a powerful magnetic field, radio frequency pulses and a computer are used to produce detailed pictures of the inside of the breasts. MRI is helpful in finding abnormalities that are not visible with mammography or ultrasound. In general, MRI is used only in women at high risk for breast cancer. For an MRI of the breast, you will lie face down on a platform with openings to accommodate your breasts and allow them to be imaged without compression. A nurse or technologist will insert an intravenous (IV) catheter, also known as an IV line, into a vein in your hand or arm. You will be moved into the magnet of the MRI unit, which is a large tunnel, and an initial set of images will be taken while you remain very still. The contrast material is injected into the intravenous line (IV) and additional images are taken. What are the benefits and risks of breast cancer screening?Mammography Benefits
Risks
Breast Ultrasound Benefits
Risks
Breast MRI Benefits
Risks
What happens if something is detected on my screening exam?Lumps, other abnormalities or questionable findings in the breast are often detected by screening tests. However, it is not always possible to tell from these imaging tests whether a finding is benign or cancerous. To determine whether there is a cancer present, your doctor may recommend that one or more of the following imaging tests may be performed:
If a finding is proven to be benign by its appearance on these exams, no further steps may need to be taken. If these tests do not clearly show that the finding is benign, a biopsy may be necessary. In a biopsy, a small amount of tissue is removed under local anesthesia so that it can be examined in a laboratory. One of the following image-guided procedures is used during a breast biopsy:
A pathologist examines the removed tissue specimen and makes a final diagnosis. Depending on the facility, the radiologist or your referring physician will share the results with you. With early detection and improved treatments, more women are surviving breast cancer. If cancer is diagnosed, your doctor will discuss your treatment options and together you will determine your course of treatment. Today, women have more treatment options than ever before. |
|
|

OPEN 24 HOURS: ACCIDENT EMERGENCY, LAB SERVICES, IMAGING SERVICES & PHARMACY